Mississippi Today
‘They try to keep people quiet’: An epidemic of antipsychotic drugs in nursing homes

Mississippi consistently ranks in the top five in the nation for its rates of antipsychotic drugging in nursing homes, data from the federal government shows.
More than one in five nursing home residents in the United States is given powerful and mind-altering antipsychotic drugs. That’s more than 10 times the rate of the general population – despite the fact that the conditions antipsychotics treat do not become more common with age.
In Mississippi, that goes up to one in four residents.
“The national average tells us that there are still a large number of older residents who are inappropriately being prescribed antipsychotics,” explained Dr. Michael Wasserman, a geriatrician and former CEO of the largest nursing home chain in California.
“The Mississippi numbers can not rationally be explained,” continued Wasserman, who has served on several panels for the federal government and was a lead delegate in the 2005 White House Conference on Aging. “They are egregious.”
The state long-term care ombudsman, Lisa Smith, declined to comment for this story.
Hank Rainer, who has worked in the nursing home industry in Mississippi as a licensed certified social worker for 40 years, said the problem is two-fold: Nursing homes not being equipped to care for large populations of mentally ill adults, as well as misdiagnosing behavioral symptoms of dementia as psychosis.
Both result in drugging the problem away with medications like antipsychotics, he said.
Antipsychotics are a special class of psychotropics designed to treat psychoses accompanied by hallucinations and paranoia, such as schizophrenia. They have also been found to be helpful in treating certain symptoms of Tourette syndrome and Huntington’s disease, two neurological diseases. All of these conditions are predominantly diagnosed in early adulthood.
The drugs come with a “black box warning,” the highest safety-related warning the Food and Drug Administration doles out, that cautions against using them in individuals with dementia. The risks of using them in patients with Alzheimer’s and other forms of dementia include death.
Yet more than a decade after a federal initiative to curb antipsychotic drugging in nursing homes began, 94% of nursing homes in Mississippi – the state with the highest rate of deaths from Alzheimer’s disease – had antipsychotic drug rates in the double digits.
Long-term care advocates and industry experts have long said that the exponentially higher number of nursing home residents on these drugs – 21% in the country and 26% in the state – is indicative of a deeper and darker problem: the substandard way America cares for its elders.
“If the nursing homes don’t have enough staff, they try to keep people quiet, so they give them sedatives or antipsychotics,” said gerontologist and nursing home expert Charlene Harrington.
And the problem, she emphasized, isn’t going away.
“Over the last 20 years we’ve had more and more corporations involved and bigger and bigger chains, and 70% are for-profit, and they’re really not in it to provide health care,” Harrington said. “… It’s a way to make money. And that’s been allowed because the state doesn’t have the money to set up their own facilities.”
‘It’s just not right to give someone a drug they don’t need’
On a late Thursday morning in August, Ritchie Anne Keller, director of nursing at Vicksburg Convalescent Center, pointed out a resident falling asleep on one of the couches on the second floor of the nursing home.
The resident, who nurses said was previously lively and would comment on the color of Keller’s scrubs every day, had just gotten back from another clinical inpatient setting where she was put on a slew of new drugs – including antipsychotics.
One or more of them may be working, Keller explained, but the nursing staff would need to eliminate the drugs and then reintroduce them, if needed, to find the path of least medication.
“How do you know which ones are helping her,” Keller asked, “when you got 10 of them?”
The home, which boasts the second-lowest rate of antipsychotic drug use in the state, is led by two women who have worked there for decades.
Keller has been at the nursing home since 1994 and entered her current position in 2004. Vicksburg Convalescent’s administrator, Amy Brown, has been at the home for over 20 years.

Low turnover and high staffing levels are two of the main reasons the home has been able to keep such a low rate of antipsychotic drug use, according to Keller. These two measures allow staff to be rigorous about meeting individual needs and addressing behavioral issues through non-medicated intervention when possible, she explained.
Keller said she often sees the effects of unnecessary drugging, and it happens because facilities don’t take the time to get to the root cause of a behavior.
“We see (residents) go to the hospital, they may be combative because they have a UTI or something, and (the hospital staff) automatically put them on antipsychotics,” she said.
Urinary tract infections in older adults can cause delirium and exacerbate dementia.
It’s important to note, said Wasserman, that Vicksburg and other Mississippi nursing homes with the lowest rates are not at zero. Medicine is always a judgment call, he argued, which is why incentivizing nursing homes to bring their rates down to 0% or even 2% could be harmful.
Schizophrenia is the only mental illness CMS will not penalize nursing home facilities for treating with antipsychotics in its quality care ratings. However, there are other FDA-approved uses, like bipolar disorder.
“As a physician, a geriatrician, I have to use my clinical judgment on what I think is going to help a patient,” Wasserman said. “And sometimes, that clinical judgment might actually have me using an antipsychotic in the case of someone who doesn’t have a traditional, FDA-approved diagnosis.”
In order to allow doctors the freedom to prescribe these drugs to individuals for whom they can drastically improve quality of life, Wasserman says the percentage of residents on antipsychotics can have some flexibility, but averages should stay in the single digits.
When 20 to 30% of nursing home residents are on these drugs, that means a large portion of residents are on them unnecessarily, putting them at risk of deadly side effects, Wasserman explained.
“But also, it’s just not right to give someone a drug they don’t need,” he said.
Experts have long said that staffing is one of the strongest predictors in quality of care – including freedom from unnecessary medication – which makes a recent federal action requiring a minimum staffing level for nursing homes a big deal.
The Biden administration finalized the first-ever national minimum staffing rule for nursing homes in April. The requirements will be phased in over two to three years for non-rural facilities and three to five years for rural facilities.
In Mississippi, all but two of the 200 skilled nursing facilities – those licensed to provide medical care from registered nurses – would need to increase staffing levels under the standards, according to data analyzed by Mississippi Today, USA TODAY and Big Local News at Stanford University.
Even Vicksburg Convalescent Center, which has a five-star rating on CMS’ Care Compare site and staffs “much above average,” will need to increase its staffing under the new regulations.
Mississippi homes with the highest antipsychotic rates
The six nursing homes with the highest antipsychotic rates in the state include three state-run nursing homes that share staff – including psychiatrists and licensed certified social workers – with the state psychiatric hospital, as well as three private, for-profit nursing homes in the Delta.
The three Delta nursing homes are Ruleville Nursing and Rehabilitation Center in Ruleville, Oak Grove Retirement Home in Duncan, and Cleveland Nursing and Rehabilitation Center in Cleveland. All have percentages of schizophrenic residents between 26 and 43%, according to CMS data.
Ruleville, a for-profit nursing home, had the highest rates of antipsychotic drugging in the state at 84% the last quarter of 2023. Slightly more than a third – or 39% – of the home’s residents had a schizophrenia diagnosis, and nearly half are 30-64 years old.
New York-based Donald Denz and Norbert Bennett own both Ruleville Nursing and Rehabilitation Center and Cleveland Nursing and Rehabilitation Center.
CMS rated the Ruleville facility as one out of five stars – or “much below average” – partly due to its rates of antipsychotic drugging.
But G. Taylor Wilson, an attorney for the nursing home, cited the facility’s high percentages of depression, bipolar and non-schizophrenic psychoses as the reason for its high rate of antipsychotic drug use, and said that all medications are a result of a physician or psychiatric nurse practitioner’s order.
While CMS has identified high antipsychotic drug rates as indicative of potential overmedication, Ruleville appears to be an exception, though it’s not clear why it accepts so many mentally ill residents or why its residents skew younger.
It is unclear what, if any, special training Ruleville staff has in caring for people with mental illness. Wilson did say the home contracts with a group specializing in psychiatric services and sends residents to inpatient and outpatient psychiatric facilities when needed.
There is no special designation or training required by the state for homes that have high populations of schizophrenic people or residents with other mental illnesses. Nursing homes must conduct a pre-admission screening to ensure they have the services needed for each admitted resident, according to the Health Department.
An official with the State Health Department, which licenses and oversees nursing homes, said there are more private nursing homes that care for people with mental illness now because of a decrease in state-run mental health services and facilities.
Agency officials pointed specifically to the closure of two nursing homes run by the Department of Mental Health after the Legislature slashed millions from the agency’s budget two years in a row.
“Due to the lack of options for many individuals who suffer from mental illness, Mississippi is fortunate that we have facilities willing to care for them,” said State Health Department Assistant Senior Deputy Melissa Parker in an emailed statement to Mississippi Today.
However, the Health Department cited Ruleville Nursing and Rehabilitation Center in May after a resident was allegedly killed by his roommate.
The resident who allegedly killed his roommate had several mental health diagnoses, according to the report. The state agency said that the facility for months neglected to provide “appropriate person-centered behavioral interventions” to him, and that this negligence caused the resident’s death and placed other residents in danger.
Wilson, the attorney for Ruleville, said his clients disagree with the state agency’s findings.
“The supposed conclusions reached by the (state agency) regarding Ruleville’s practices are not fact; they are allegations which Ruleville strongly disputes,” he said.
Oversight of nursing homes is limited
In 2011, U.S. Inspector General Daniel Levinson said “government, taxpayers, nursing home residents, as well as their families and caregivers should be outraged – and seek solutions” in a brief following an investigative report that kickstarted the movement against overprescription of antipsychotics in nursing homes.
“It was pretty striking,” said Richard Mollot, executive director of the Long Term Care Community Coalition, a nonprofit advocacy group dedicated to improving the lives of elderly and disabled people in residential facilities. “The Office of the Inspector General … They’re pretty conservative people. They don’t just come out and say that the public should be outraged by something.”
That landmark report showed that 88% of Medicare claims for atypical antipsychotics – the primary class of antipsychotics used today – were for residents diagnosed with dementia. The black box warning cautioning against use in elderly residents with dementia was introduced six years earlier in 2005.
But the problem persists today – and experts cite lack of oversight as one of the leading causes.
“CMS has had that whole initiative to try to reduce antipsychotics, and it’s been 10 years, and basically, they’ve had no impact,” Harrington said. “Partly because they’re just not enforcing it. Surveyors are not giving citations … So, the practice just goes on.”

In Mississippi, 52 nursing homes were cited 55 times in the last five years for failing to keep elderly residents free of unnecessary psychotropics, according to State Health Department data.
Barring specific complaints of abuse, nursing homes are generally inspected once a year, according to the State Health Department. In Mississippi, 54% of nursing home state surveyor positions were vacant in 2022, and 44% of the working surveyors had less than two years of experience.
During an inspection, a sample group usually consisting of three to five residents is chosen based on selection from surveyors and the computer system. That means if a nursing home is cited for a deficiency affecting one resident, that’s one resident out of the sample group – not one resident in the entire facility.
The state cited Bedford Care Center of Marion in 2019 for unnecessarily administering antipsychotics. The inspection report reveals that four months after a resident was admitted to the facility, he was prescribed an antipsychotic for “dementia with behaviors.”
The resident’s wife said her husband started sleeping 20 hours a day after starting the medication, according to the inspection report, yet the nursing home continued to administer the drug at the same dose for six months.
CMS mandates that facilities attempt to reduce dose reductions for residents on psychotropic drugs and incorporate behavioral interventions in an effort to discontinue these drugs, unless clinically contraindicated.
The facility did not respond to a request for comment from Mississippi Today.
In another instance, Ocean Springs Health and Rehabilitation Center was cited in 2019 after the facility’s physician failed to decrease three residents’ medications as a pharmacy consultant had recommended. The inspection report says there was no documentation as to why.
Officials with the nursing home did not respond to a request for comment from Mississippi Today.
These two incidents – and all citations for this deficiency in the last five years – were cited as “level 2,” meaning “no actual harm” as defined by federal guidelines. Facilities are not fined for these citations, and their quality care score is only minimally impacted.
“If they don’t say there’s harm, then they can’t give a fine,” Harrington said. “And even when they do give fines, they’re usually so low they have no effect. A $3,000 fine is just the cost of doing business. They don’t pay any attention to it.”
“Level 3” and “Level 4” are mostly used in extreme and unlikely situations, explained Angela Carpenter, director of long-term care at the State Health Department.
“For example,” she said, a Level 4 would be “if a person was placed on Haldol (an antipsychotic), he began having seizures, they still continued to give him the Haldol, they didn’t do a dose reduction, and the person ended up dying of a heart attack with seizures when they didn’t have a seizure disorder.”
“Actual harm” is supposed to also include psychosocial harm, according to federal guidelines, but Carpenter said psychosocial harm “can be very difficult to prove,” as it involves going back to the facility and doing multiple interviews to figure out what the individual was like before the drugs – not to mention many symptoms are attributed to the cognitive decline associated with the aging process instead of being seen as possible symptoms of medication.
Experts say the bar for “harm” is far too high.
“And that sends a message that ‘Well, you know, we gave them a drug that changes the way their brain works, and we did it unnecessarily, but you know, no harm’ – and that’s where I think the regulators really don’t have a good understanding of what is actually happening here,” said Tony Chicotel, an elder attorney in California.
‘Looking at the person as a whole’: More humane solutions
Hank Rainer, a licensed certified social worker, has worked in Mississippi nursing homes for decades. Nursing homes contract with him to train social services staff in how best to support residents and connect them with services they need.
Rainer believes there are several solutions to mitigating the state’s high rates of antipsychotic drugs. Those include training more physicians in geriatrics, increasing residents’ access to psychiatrists and licensed certified social workers, and creating more memory care units that care for people with dementia.
The nation is currently facing a severe shortage of geriatricians, with roughly one geriatrician for every 10,000 older patients. The American Geriatrics Society estimates one geriatrician can care for about 700 patients.
Because it’s rare for a nursing home to contract with a psychiatrist, most residents are prescribed medication – including for mental health disorders – by a nurse practitioner or family medicine doctor, neither of which have extensive training in psychiatry or geriatrics.
Rainer also said having more licensed certified social workers in nursing homes would better equip homes to address residents’ issues holistically.
“LCSWs are best suited to help manage behaviors in nursing homes and other settings, as they look at the person as a whole,” he said. “They don’t just carve out and treat a disease. They look at the person’s illness and behaviors in regard to the impact of environmental, social and economic influences as well as the physical illness.”
That’s not to say, he added, that some residents might not benefit most from pharmacological interventions in tandem with behavioral interventions.
Finally, creating more memory care units that have the infrastructure to care for dementia behaviors with non-medicated intervention is especially important, Rainer said, given the fact that antipsychotics not only do not treat dementia, but also pose a number of health risks to this population.
Dementia behaviors are often mistaken for psychosis, Rainer said, and having trained staff capable of making the distinction can be lifesaving. He gave an example of an 85-year-old woman with dementia who kept asking for her father.
The delusion that her father was still alive technically meets the criteria for psychosis, he said, and so untrained staff may think antipsychotic medication was an appropriate treatment.
However, trained staff would know how to implement interventions like meaningful diversional activities or validation therapy prior to the use of medications, he continued.
“The father may represent safety and they may not feel safe in the building because they don’t know anyone there,” Rainer said. “Or the father may represent home and security and warmth and they may not feel quite at home in the facility. You don’t ever agree that their dad is coming to get them. That is not validation therapy. But what you do is you try to key in under the emotional component and get them to talk about that, and redirect them at the same time.”
With more people living longer with conditions such as Alzheimer’s, good dementia care is becoming increasingly more important.
But first the nursing homes would need to find the staff, Chicotel said.
As it stands, with the vast majority of nursing homes in the country staffing below expert recommendations – nearly all nursing homes would have to increase staffing under not-yet-implemented Biden regulations, which are less stringent than federal recommendations made in 2001 – non-pharmacological, resident-centered care is hard to come by.
“Trying to anticipate needs in advance and meeting them, spending more time with people so they don’t feel so uncomfortable and distressed and scared – that’s a lot of human touch that unfortunately is a casualty when facilities are understaffed,” Chicotel explained.
Help us continue to report on Mississippi’s nursing homes by taking the survey below.
This article first appeared on Mississippi Today and is republished here under a Creative Commons license.![]()
Mississippi Today
On this day in 1898

Feb. 22, 1898

Frazier Baker, the first Black postmaster of the small town of Lake City, South Carolina, and his baby daughter, Julia, were killed, and his wife and three other daughters were injured when a lynch mob attacked.
When President William McKinley appointed Baker the previous year, local whites began to attack Baker’s abilities. Postal inspectors determined the accusations were unfounded, but that didn’t halt those determined to destroy him.
Hundreds of whites set fire to the post office, where the Bakers lived, and reportedly fired up to 100 bullets into their home. Outraged citizens in town wrote a resolution describing the attack and 25 years of “lawlessness” and “bloody butchery” in the area.
Crusading journalist Ida B. Wells wrote the White House about the attack, noting that the family was now in the Black hospital in Charleston “and when they recover sufficiently to be discharged, they) have no dollar with which to buy food, shelter or raiment.
McKinley ordered an investigation that led to charges against 13 men, but no one was ever convicted. The family left South Carolina for Boston, and later that year, the first nationwide civil rights organization in the U.S., the National Afro-American Council, was formed.
In 2019, the Lake City post office was renamed to honor Frazier Baker.
“We, as a family, are glad that the recognition of this painful event finally happened,” his great-niece, Dr. Fostenia Baker said. “It’s long overdue.”
This article first appeared on Mississippi Today and is republished here under a Creative Commons license.![]()
Mississippi Today
Memorial Health System takes over Biloxi hospital, what will change?

by Justin Glowacki with contributions from Rasheed Ambrose, Javion Henry, McKenna Klamm, Matt Martin and Aidan Tarrant
BILOXI – On Feb. 1, Memorial Health System officially took over Merit Health Biloxi, solidifying its position as the dominant healthcare provider in the region. According to Fitch Ratings, Memorial now controls more than 85% of the local health care market.
This isn’t Memorial’s first hospital acquisition. In 2019, it took over Stone County Hospital and expanded services. Memorial considers that transition a success and expects similar results in Biloxi.
However, health care experts caution that when one provider dominates a market, it can lead to higher prices and fewer options for patients.
Expanding specialty care and services

One of the biggest benefits of the acquisition, according to Kristian Spear, the new administrator of Memorial Hospital Biloxi, will be access to Memorial’s referral network.
By joining Memorial’s network, Biloxi patients will have access to more services, over 40 specialties and over 100 clinics.
“Everything that you can get at Gulfport, you will have access to here through the referral system,” Spear said.
One of the first improvements will be the reopening of the Radiation Oncology Clinic at Cedar Lake, which previously shut down due to “availability shortages,” though hospital administration did not expand on what that entailed.
“In the next few months, the community will see a difference,” Spear said. “We’re going to bring resources here that they haven’t had.”
Beyond specialty care, Memorial is also expanding hospital services and increasing capacity. Angela Benda, director of quality and performance improvement at Memorial Hospital Biloxi, said the hospital is focused on growth.
“We’re a 153-bed hospital, and we average a census of right now about 30 to 40 a day. It’s not that much, and so, the plan is just to grow and give more services,” Benda said. “So, we’re going to expand on the fifth floor, open up more beds, more admissions, more surgeries, more provider presence, especially around the specialties like cardiology and OB-GYN and just a few others like that.”
For patient Kenneth Pritchett, a Biloxi resident for over 30 years, those changes couldn’t come soon enough.

Pritchett, who was diagnosed with congestive heart failure, received treatment at Merit Health Biloxi. He currently sees a cardiologist in Cedar Lake, a 15-minute drive on the interstate. He says having a cardiologist in Biloxi would make a difference.
“Yes, it’d be very helpful if it was closer,” Pritchett said. “That’d be right across the track instead of going on the interstate.”
Beyond specialty services and expanded capacity, Memorial is upgrading medical equipment and renovating the hospital to improve both function and appearance. As far as a timeline for these changes, Memorial said, “We are taking time to assess the needs and will make adjustments that make sense for patient care and employee workflow as time and budget allow.”
Unanswered questions: insurance and staffing
As Memorial Health System takes over Merit Health Biloxi, two major questions remain:
- Will patients still be covered under the same insurance plans?
- Will current hospital staff keep their jobs?
Insurance Concerns
Memorial has not finalized agreements with all insurance providers and has not provided a timeline for when those agreements will be in place.
In a statement, the hospital said:
“Memorial recommends that patients contact their insurance provider to get their specific coverage questions answered. However, patients should always seek to get the care they need, and Memorial will work through the financial process with the payers and the patients afterward.”
We asked Memorial Health System how the insurance agreements were handled after it acquired Stone County Hospital. They said they had “no additional input.”
What about hospital staff?
According to Spear, Merit Health Biloxi had around 500 employees.
“A lot of the employees here have worked here for many, many years. They’re very loyal. I want to continue that, and I want them to come to me when they have any concerns, questions, and I want to work with this team together,” Spear said.
She explained that there will be a 90-day transitional period where all employees are integrated into Memorial Health System’s software.
“Employees are not going to notice much of a difference. They’re still going to come to work. They’re going to do their day-to-day job. Over the next few months, we will probably do some transitioning of their computer system. But that’s not going to be right away.”
The transition to new ownership also means Memorial will evaluate how the hospital is operated and determine if changes need to be made.
“As we get it and assess the different workflows and the different policies, there will be some changes to that over time. Just it’s going to take time to get in here and figure that out.”
During this 90-day period, Erin Rosetti, Communications Manager at Memorial Health System said, “Biloxi employees in good standing will transition to Memorial at the same pay rate and equivalent job title.”
Kent Nicaud, President and CEO of Memorial Health System, said in a statement that the hospital is committed to “supporting our staff and ensuring they are aligned with the long-term vision of our health system.”
What research says about hospital consolidations
While Memorial is promising improvements, larger trends in hospital mergers raise important questions.
Research published by the Rand Corporation, a nonprofit, nonpartisan research organization, found that research into hospital consolidations reported increased prices anywhere from 3.9% to 65%, even among nonprofit hospitals.
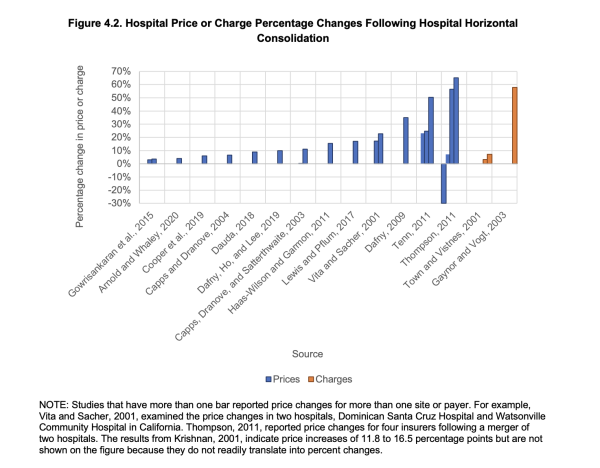
The impact on patient care is mixed. Some studies suggest merging hospitals can streamline services and improve efficiency. Others indicate mergers reduce competition, which can drive up costs without necessarily improving care.
When asked about potential changes to the cost of care, hospital leaders declined to comment until after negations with insurance companies are finalized, but did clarify Memorial’s “prices are set.”
“We have a proven record of being able to go into institutions and transform them,” said Angie Juzang, Vice President of Marketing and Community Relations at Memorial Health System.
When Memorial acquired Stone County Hospital, it expanded the emergency room to provide 24/7 emergency room coverage and renovated the interior.
When asked whether prices increased after the Stone County acquisition, Memorial responded:
“Our presence has expanded access to health care for everyone in Stone County and the surrounding communities. We are providing quality healthcare, regardless of a patient’s ability to pay.”
The response did not directly address whether prices went up — leaving the question unanswered.
The bigger picture: Hospital consolidations on the rise
According to health care consulting firm Kaufman Hall, hospital mergers and acquisitions are returning to pre-pandemic levels and are expected to increase through 2025.
Hospitals are seeking stronger financial partnerships to help expand services and remain stable in an uncertain health care market.
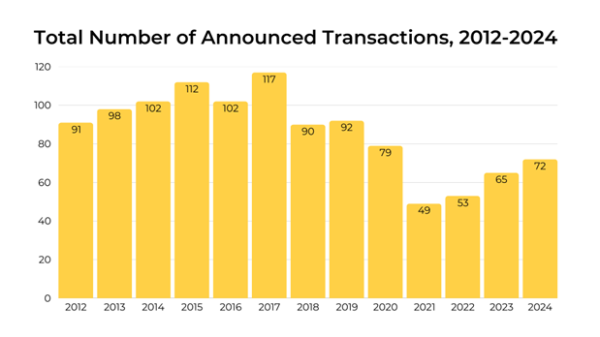
Source: Kaufman Hall M&A Review
Proponents of hospital consolidations argue mergers help hospitals operate more efficiently by:
- Sharing resources.
- Reducing overhead costs.
- Negotiating better supply pricing.
However, opponents warn few competitors in a market can:
- Reduce incentives to lower prices.
- Slow wage increases for hospital staff.
- Lessen the pressure to improve services.
Leemore Dafny, PhD, a professor at Harvard and former deputy director for health care and antitrust at the Federal Trade Commission’s Bureau of Economics, has studied hospital consolidations extensively.
In testimony before Congress, she warned: “When rivals merge, prices increase, and there’s scant evidence of improvements in the quality of care that patients receive. There is also a fair amount of evidence that quality of care decreases.”
Meanwhile, an American Hospital Association analysis found consolidations lead to a 3.3% reduction in annual operating expenses and a 3.7% reduction in revenue per patient.
This article first appeared on Mississippi Today and is republished here under a Creative Commons license.![]()
Mississippi Today
Adopted people face barriers obtaining birth certificates. Some lawmakers point to murky opposition from judges

When Judi Cox was 18, she began searching for her biological mother. Two weeks later she discovered her mother had already died.
Cox, 41, was born in Gulfport. Her mother was 15 and her father didn’t know he had a child. He would discover his daughter’s existence only when, as an adult, she took an ancestry test and matched with his niece.
It was this opaque family history, its details coming to light through a convergence of tragedy and happenstance, that led Cox to seek stronger legal protections for adopted people in Mississippi. Ensuring adopted people have access to their birth certificates has been a central pillar of her advocacy on behalf of adoptees. But legislative proposals to advance such protections have died for years, including this year.
Cox said the failure is an example of discrimination against adopted people in Mississippi — where adoption has been championed as a reprieve for mothers forced into giving birth as a result of the state’s abortion ban.
“A lot of people think it’s about search and reunion, and it’s not. It’s about having equal rights. I mean, everybody else has their birth certificate,” Cox said. “Why should we be denied ours?”
Mississippi lawmakers who have pushed unsuccessfully for legislation to guarantee adoptees access to their birth certificate have said, in private emails to Cox and interviews with Mississippi Today, that opposition comes from judges.
“There are a few judges that oppose the bill from what I’ve heard,” wrote Republican Sen. Angela Hill in a 2023 email.
Hill was recounting opposition to a bill that died during the 2023 legislative session, but a similar measure in 2025 met the same fate. In an interview this month, Hill said she believed the political opposition to the legislation could be bound up with personal interest.
“Somebody in a high place doesn’t want an adoption unsealed,” Hill said. “I don’t know who we’re protecting from somebody finding their birth parents,” Hill said. “But it leads you to believe some people have a very strong interest in keeping adoption records sealed. Unless it’s personal, I don’t understand it.”
In another 2023 email to Cox reviewed by Mississippi Today, Republican Rep. Lee Yancey wrote that some were concerned the bill “might be a deterrent to adoption if their identities were disclosed.”
The 2023 legislative session was the first time a proposal to guarantee adoptees access to their birth certificates was introduced under the state’s new legal landscape surrounding abortion.
In 2018, Mississippi enacted a law that banned most abortions after 15 weeks. The state’s only abortion clinic challenged the law, and that became the case that the U.S. Supreme Court used in 2022 to overturn Roe v. Wade, its landmark 1973 ruling that established a nationwide right to abortion.
Roe v. Wade had rested in part on a woman’s right to privacy, a legal framework Mississippi’s Solicitor General successfully undermined in Dobbs v. Jackson Women’s Health Organization. Before that ruling, anti-abortion advocates had feared allowing adoptees to obtain their birth certificates could push women toward abortion rather than adoption.
Abortion would look like a better option for parents who feared future contact or disclosure of their identities, the argument went. With legal access to abortion a thing of the past in Mississippi, Cox said she sees a contradiction.
“Mississippi does not recognize privacy in that matter, as far as abortions and all that. So if you don’t acknowledge it in an abortion setting, how can you do it in an adoption setting?” Cox said. “You can’t pick and choose whether you’re going to protect my privacy.”
Opponents to legislation easing access to birth certificates for adoptees have also argued that such proposals would unfairly override previous affidavits filed by birth parents requesting privacy.
The 2025 bill, proposed by Republican Rep. Billy Calvert, would direct the state Bureau of Vital Records to issue adoptees aged 21 and older a copy of their original birth certificate.
The bill would also have required the Bureau to prepare a form parents could use to indicate their preferences regarding contact from an adoptee. That provision, along with existing laws that guard against stalking, would give adoptees access to their birth certificate while protecting parents who don’t wish to be contacted, Cox said.
In 2021, Cox tried to get a copy of her birth certificate. She asked Lauderdale County Chancery Judge Charlie Smith, who is now retired, to unseal her adoption records. The Judge refused because Cox had already learned the identity of her biological parents, emails show.
“With the information that you already have, Judge Smith sees no reason to grant the request to open the sealed adoption records at this time,” wrote Tawanna Wright, administrator for the 12th District Chancery Court in Meridian. “If you would like to formally file a motion and request a hearing, you are certainly welcome to do so.”
In her case and others, judges often rely on a subjective definition of what constitutes a “good cause” for unsealing records, Cox said. Going through the current legal process for unsealing records can be costly, and adoptees can’t always control when and how they learn the identity of their biological parents, Cox added.
After Cox’s biological mother died, her biological uncle was going through her things and came across the phone number for Cox’s adoptive parents. He called them.
“My adoptive mom then called to tell me the news — just hours after learning I was expecting my first child,” Cox said.
This article first appeared on Mississippi Today and is republished here under a Creative Commons license.![]()
-

 News from the South - Louisiana News Feed2 days ago
News from the South - Louisiana News Feed2 days agoJeff Landry’s budget includes cuts to Louisiana’s domestic violence shelter funding
-

 News from the South - North Carolina News Feed6 days ago
News from the South - North Carolina News Feed6 days agoModest drops in some North Carolina prices under Trump | North Carolina
-

 News from the South - Texas News Feed7 days ago
News from the South - Texas News Feed7 days agoA developer bought up 70 properties on a historically Black street. The community doesn't know what's next
-

 News from the South - Arkansas News Feed6 days ago
News from the South - Arkansas News Feed6 days agoTiming out the incoming winter weather
-

 News from the South - Arkansas News Feed7 days ago
News from the South - Arkansas News Feed7 days agoFrigid Sunday conditions in Northwest Arkansas
-

 News from the South - Oklahoma News Feed4 days ago
News from the South - Oklahoma News Feed4 days agoRemains of Aubrey Dameron found, family gathers in her honor
-

 News from the South - Kentucky News Feed7 days ago
News from the South - Kentucky News Feed7 days agoEight die in flooding across Kentucky as rescues continue, governor warns of ‘wild weather week’
-

 News from the South - Florida News Feed6 days ago
News from the South - Florida News Feed6 days agoExpert discusses how deportations could cause labor shortages for several industries











































