Matthew Hatcher/AFP via Getty Images
Kimberly Dodd, Michigan State University
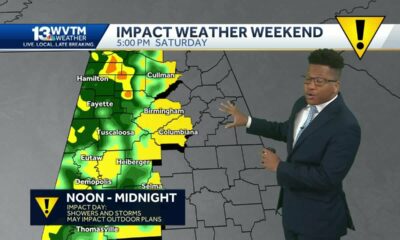
After a relatively quiet fall, there’s been another spike in cases of bird flu in Michigan.
When state officials announced on Dec. 16, 2024, that bird flu had been found in another poultry facility in Ottawa County, it was the first time the H5N1 virus had been detected in Michigan poultry in over six months. Since then, the U.S. Department of Agriculture has confirmed seven more outbreaks – in five commercial and two backyard flocks – in the state, the most recent in Oakland County.
Meanwhile, on Jan. 6, 2025, the Centers for Disease Control and Prevention reported the first human death from bird flu in the U.S., in Louisiana.
Bird flu is a complex and evolving disease with significant impact to the poultry and dairy industries. Since the beginning of the outbreaks in poultry and cattle, almost 135 million birds and more than 900 cattle herds have been affected nationwide. A significant number of wild animals – such as raccoon, skunks, foxes and bobcats – as well as marine mammals and domestic cats have also died from the virus.
Kimberly Dodd, dean of Michigan State University’s College of Veterinary Medicine, is an expert in outbreak response for emerging infectious diseases. Michigan was among the first states to see H5N1 outbreaks in commercial poultry and dairy facilities. Both state and federal officials have worked closely with the Michigan State University Veterinary Diagnostic Laboratory to identify newly infected herds, while continuing to provide surveillance for the virus in poultry and wild birds.
Dodd talked to The Conversation U.S. about the risks H5N1 presents to families, pets and livestock, and how researchers are working together to find ways to limit its spread.
What are Michigan researchers learning about the outbreak?
In the case of H5N1 in cows, scientists and animal health experts here in Michigan and around the country are working to understand a familiar disease in a novel species.
The transmission of the avian flu virus H5N1 to dairy cattle was first confirmed in March 2024 in Texas and has since spread to 15 other U.S. states, most recently California.
The virus impacts milk production and poses significant risks to other bird species, particularly domestic poultry as well as some mammals. The CDC has also confirmed mild cases in humans, and a fatal one in Louisiana in January 2025.
Diagnosticians at Michigan State University and the USDA’s National Animal Health Laboratory Network provide rapid diagnostics to identify infected herds and monitor the virus in wild birds and mammals, helping control the spread.
We’ve learned, based on sequencing the circulating viruses, that there is a specific virus strain or H5N1 genotype, B3.13, circulating in cows and poultry. Subtle changes over time in the genetic makeup of the virus points to a single spillover event. This means the virus likely spread from wild birds to a cow in Texas, and then spread from cow to cow. We also know that there is a separate H5N1 genotype, D1.1, that is currently circulating in wild birds and domestic poultry.
Researchers in our College of Veterinary Medicine are working with federal and state officials and farmers to determine how long cows produce infectious milk. The goal is to understand how cows are becoming infected within and across herds so that we can better mitigate the spread.

Justin Sullivan/Getty Images
Why is it called bird flu if it sickens other animals too?
Influenza viruses affect many animals including humans, pigs, dogs and horses.
There are four types of influenza viruses: A, B, C and D, which are loosely defined by the species they can infect. Avian influenza viruses are considered influenza A viruses. Interestingly, influenza D viruses are the ones that primarily infect cattle. But the current H5N1 circulating in dairy cattle is the same influenza A virus as seen in the ongoing outbreak in birds.
This is of particular concern, as only influenza A viruses have been associated with human pandemics.
Avian influenza viruses circulate in wild birds but don’t typically cause them significant disease. While many avian influenza viruses can infect poultry, their behavior in those hosts classifies the virus as either highly pathogenic or low pathogenic. It’s important to note that this classification doesn’t necessarily indicate how easily it spreads or the likelihood that the virus will jump to other species.
The currently circulating strain is classified as highly pathogenic avian influenza, or HPAI, based on the high mortality it causes domestic poultry. One of the many unusual characteristics of the current outbreak is the high mortality seen in wild birds; as a result, we have seen many species of young carnivores and scavengers infected by the virus.
Infection in other species often requires exposure to a large amount of virus, or a compromised or underdeveloped immune system. These are typically “dead-end hosts.” They become infected but do not play a role in virus spread because either the animal dies or it becomes infected but not infectious.
The current outbreak of HPAI H5N1 has been ongoing since 2021. The outbreak is notable for its duration, wide geographic spread and unusual impact on nonpoultry species as well. It has caused significant illness and death in wild birds like ducks and geese, as well as mammals exposed to infected bird carcasses like cats and skunks.
However when the USDA unexpectedly confirmed that H5N1 was the cause of significant disease in dairy cattle in early 2024, it marked the first time that the virus was detected in U.S. dairy cattle.
What does the virus do to cattle?
Most cows infected with H5N1 recover on their own without treatment. Symptoms include fever and sluggishness. There is also decreased appetite and a significant drop in milk production in lactating cows, as the virus is concentrated in the mammary glands and milk.
There are three reasons to care about the ongoing H5N1 outbreak in dairy cattle:
First, the drop in milk production and the virus’s infectious nature create challenges for farmers to control the infection and lead to economic losses. In addition to the production losses, there are additional labor and supply costs to manage the outbreak in the herd, including separation and supportive care of sick cows. Workers also need to use personal protective equipment to prevent spread of the virus to healthy animals and to protect themselves from potential infection.
Second, dairy cows produce large amounts of the virus in milk, which is highly infectious. While pasteurization kills the virus, raw milk remains a major infection risk. Significant numbers of wild mammals and domestic cats on dairy farms have died from the virus after consuming raw milk. It also poses a risk to dairy workers.
The virus has also spread from dairy farms to poultry facilities, causing high bird mortality. Experts are exploring the possibility that clothing, shoes, trucks, equipment and other items that have been contaminated with raw milk containing the virus can lead to inadvertent, and lethal, exposure for poultry.
Third, prolonged circulation in cattle increases the risk of the virus adapting to mammals, including humans.
To monitor this risk, all H5N1-positive samples are sent to the USDA for genetic sequencing to identify mutations that may increase the virus’s ability to infect mammals and to provide important information about how the virus spreads within and between populations.
How do we manage H5N1 moving forward?
Biosecurity for poultry and dairy facilities is more critical than ever. Biosecurity measures include limiting visitors to farms and facilities; disinfecting tools, footwear and equipment; avoiding contact between infected and noninfected species; and isolating sick animals.
These measures play an important role in both containing the virus and keeping it away from other animals, properties and people.![]()
Kimberly Dodd, Dean of College of Veterinary Medicine, Michigan State University
This article is republished from The Conversation under a Creative Commons license. Read the original article.